Chronic Lymphocytic Leukemia is a condition chronic lymphocytic leukemia is a variation of leukemia that is commonly seen in adults. Most patients diagnosed with this condition may live up to 5- 10 years but those that have developed complications may only live for around 2-3 years [1, 2].
What is Chronic Lymphocytic Leukemia?
Chronic lymphocytic leukemia (CLL) is a type of leukemia where the bone marrow produces abnormal lymphocytes which are not able to function properly. Normally, the bone marrow produces hematopoietic stem cells that may become a red blood cell, white blood cell or platelets. In an individual diagnosed with CLL, most of the blood cells become abnormal lymphocytes and they do not turn into healthy white blood cells. These abnormal cells continues to divide and proliferate and leave little room for the normal cells to develop. A high number of lymphocytes may result in low numbers of other blood cells such as red blood cells and platelets [3, 4].
Staging
Staging of CLL is done to describe the spread of the malignancy in the body. According to the Rai system, there are 5 stages of CLL [5].
Stage 0
There is increased production of lymphocytes but there is no enlargement of the lymph nodes [5].
Stage I
Aside from the increased number of lymphocytes, the lymph nodes have enlarged as well. There number of blood cells are near the normal level and the spleen is still normal in size [5].
Stage II
Lymphocytosis is combined with the enlargement of spleen and possibly the liver. The blood count are near normal levels as well [5].
Stage III
The patient will present with anemia or low red blood cell count. There are no enlargement of lymph nodes and the platelet count is near the normal level [5].
Stage IV
The lymphocytosis is combined with thrombocytopenia or low platelet count. Patients with this type of CLL may have anemia or enlargement of the lymph nodes and spleen [5].
Causes
Doctors have not yet identified the exact cause of CLL but it has been associated to genetic errors. These mutations cause the bone marrow to produce the abnormal blood cells. These lymphocytes are ineffective and continuously divide. They accumulate in the bone marrow and leave little space for normal blood cells to grow. They may also spread to other organs and cause complications [4, 5].
Risk Factors
Age – Majority of individuals who are diagnosed with CLL are over 60 years of age [1, 3, 4].
Race – White people are more likely to develop CLL than any other races [1, 3, 4].
Familial history – Having an individual who have developed CLL or any bone marrow cancer in the family increases the risk [1, 3, 4].
Chemical exposure – The use of insecticides and herbicides have been linked to the development of CLL [1, 3, 4].
Signs and Symptoms
Patients who have been diagnosed with CLL have a low number of normal white blood cells and this may result in frequent bouts of infections. Lymph nodes in the groin, armpits and neck area may develop. The lack of red blood cells may cause anemia and symptoms such as tiredness, breathlessness and easy fatigability. The low number of platelets may lead to easy bruising or bleeding. A painful lump may develop in the left side of the abdomen due to the enlargement of the spleen. Other symptoms that may be present include night sweats and unexplained weight loss [1, 3, 4].
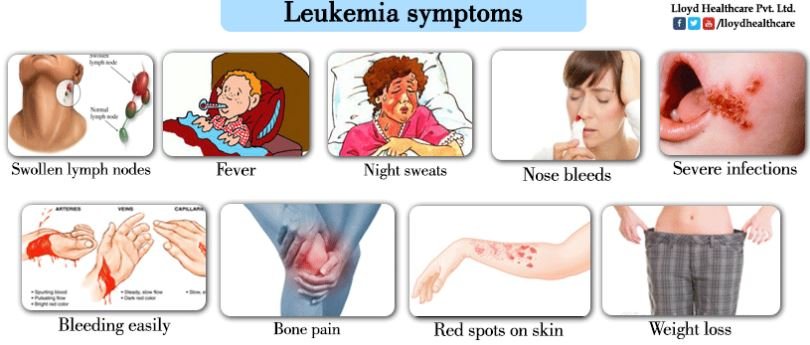
Image 1 – Symptoms of CLL
Diagnosis
Health history and physical examination
The physician will elicit a health history and it will include information about any past illnesses or health problems. The time when the symptoms started appearing will be known as well. In the physical examination, the presence of any swollen lymph nodes or increase in size of the spleen will be assessed [1, 4, 6].
Complete blood count with differential
A blood sample will be obtained from the patient and its components will be analyzed. This test will be able to show the extent of the decrease in the number of blood cells [1, 4, 6].
Bone marrow aspiration and biopsy
A sample of the bone marrow will be examined under a microscope. This test will show the presence of abnormal blood cells because of the tendency of the lymphocytes to proliferate in the bone marrow [1, 4, 6].
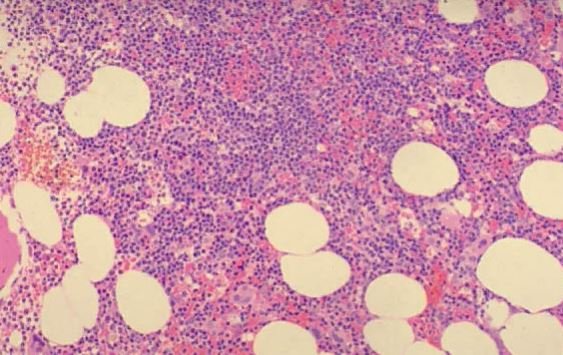
Image – CLL (observe infiltration with small, mature-appearing lymphocytes)
Treatment
The treatment for CLL is not given during the early stages of the disease because of the potential side effects that are associated with the treatment. Physicians monitor the condition of the patient and reserve the treatment for when the condition progresses. The different modes of treatment that are used are as follows [3, 4].
Chemotherapy
This cancer treatment inhibit the growth of cancer by either stopping them from multiplying or eliminating them. The combination of the drugs to be used and the method of administration depends on the progression of the disease condition. After undergoing this treatment, the patient may also have a splenectomy or removal of the enlarged spleen [3, 4].
Targeted therapy
Targeted therapy also uses drugs but its effect is selective to the cancer cells. Unlike chemotherapy, this regimen does not harm normal cells. Examples under this category include are tyrosine kinase inhibitors therapy and monoclonal antibodies therapy [3, 4].
Biologic therapy
In biologic therapy, the patient’s own immune system is used to destroy the leukemia cells in the body. Substances that are either produced by the body or synthesized in a laboratory are utilized to boost the immune system. This treatment is also known as immunotherapy or biotherapy [3, 4].
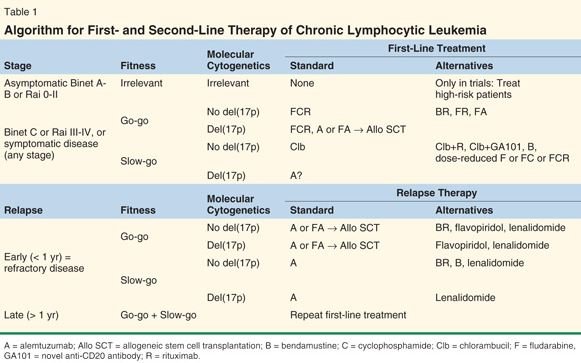
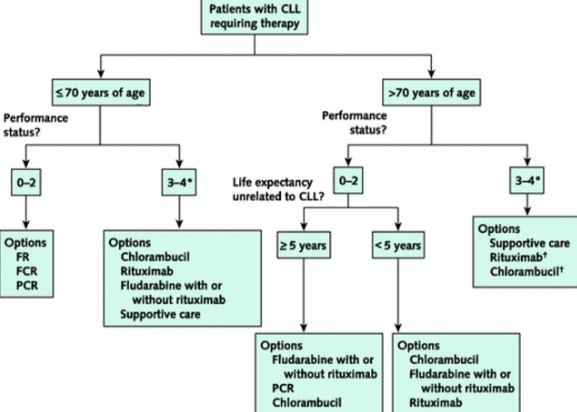
Image 4 – 1st and 2nd line therapy of CLL
Life expectancy, Prognosis, Survival Rate
Studies done on patients with CLL showed that around 60% of the patients survived after 5 years of being diagnosed while about 34% are still living after 10 years. Those with a slow-growing variation of the condition may survive longer than those with aggressive type. Factors which may contribute to a negative prognosis are old age and increased levels of beta-2-microglobulin in their blood. On the other hand, those with a non-diffuse pattern of CLL have a more positive outcome. Genetic changes such as deletion of a part of chromosome 13 in leukemic cells are associated with a better prognosis.
References
- Mir, M. A. (2016, May 23). Chronic Lymphocytic Leukemia. Retrieved from eMedicine: http://emedicine.medscape.com/article/199313-overview
- National Cancer Institute. (2015, October 23). Chronic Lymphocytic Leukemia Treatment (PDQ®)–Patient Version. Retrieved from National Cancer Institute: http://www.cancer.gov/types/leukemia/patient/cll-treatment-pdq
- Robinson, J. (2014, September 14). Chronic Lymphocytic Leukemia. Retrieved from Web MD: http://www.webmd.com/cancer/lymphoma/chronic-lymphocytic-leukemia-rare
- Mayo Clinic Staff. (2016, April 19). Chronic lymphocytic leukemia. Retrieved from Mayo Clinic: http://www.mayoclinic.org/diseases-conditions/chronic-lymphocytic-leukemia/home/ovc-20200671
- American Cancer Society. (2016, February 23). What is chronic lymphocytic leukemia? Retrieved from American Cancer Society: http://www.cancer.org/cancer/leukemia-chroniclymphocyticcll/detailedguide/leukemia-chronic-lymphocytic-what-is-cll
- Macmillan Cancer Support. (2016). Chronic Lymphocytic Leukemia. Retrieved from Macmillan Cancer Support: http://www.macmillan.org.uk/information-and-support/leukaemia/chronic-lymphocytic/diagnosing/how-cancers-are-diagnosed/tests-and-scans
Similar Posts:
- Acute Lymphocytic Leukemia
- Childhood Leukemia
- Chronic Myelogenous Leukemia
- Acute Myeloid Leukemia
- Acute Lymphoblastic Leukemia
- Mast Cell Tumor
- Non Hodgkin’s lymphoma – Symptoms, Survival Rate, Treatment, Prognosis






Leave a Reply