What is Pleomorphic Adenoma ?
Pleomorphic adenoma, also referred to as benign mixed tumors (BMTs), is a benign or a non-cancerous growth in the salivary gland, the most commonly occurring parotid tumor.
The epidemiology of pleomorphic adenoma can cover all ages and both genders but is more prevalent among women from thirty to sixty years of age. From its name, pleomorphic depicts variability in its morphology. Its diverse cytologic presentation involves epithelial, myoepithelial or salivary contractile tissues and mesenchymal components.
Epithelial gives the polygon-like squamous presentation, myoepithelial are spindle-shaped and the mesenchymal or stromal component gives the neoplasm mucoid cartilaginous form.
Pleomorphic adenoma can thrive in any of the salivary gland areas but are most commonly located in the parotid gland. The tumor presents as a single, well-defined growth, usually found in the palatine process and lips.
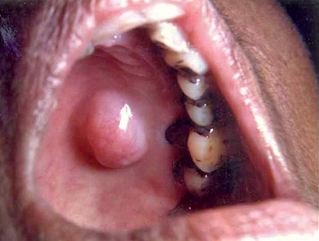
Pleomorphic adenoma presenting a 2x2cm well circumscribed lesion on the palate of a 67-year old female (IARC Screening Group. International Agency for Research on Cancer WHO).
Pleomorphic Adenoma Symptoms
Pleomorphic adenoma usually develops as a nontender nodular lesion with a slow growth rate persisting for years. Manifestations vary depending on the primary location of proliferation. The lesions are movable except for those in the palate.
Sublingual tumor presents with fullness in the oral mucosal floor. Minor glands involvement is characterized by difficulty chewing and painless swelling under the cheek and palatine processes.
Laryngeal location leads to airway obstruction, lump in the throat, disturbance in breathing, voice hoarseness, and dysphagia or difficulty swallowing. Nasal and paranasal tissue affectation may include complaints of epistaxis, nasal obstruction and sinusitis. For larger parotid tumor, facial paralysis or weakness could occur as a result of facial nerve compression.
Long-term growth commonly leads to blockage of the ducts of the salivary glands. In partial obstruction, the patient experiences swelling and feels uncomfortable especially after meals, whereas in complete obstruction, nagging pain of the gland is felt worsened by eating.
Although non-cancerous or benign in classification, it has the potential to massively extend to adjacent tissues and transform into salivary gland malignancies like carcinoma ex-pleomorphic adenoma and adenoid cystic carcinoma.
Pleomorphic Adenoma Causes
The established primary cause of pleomorphic adenoma is the failure to adequately drain saliva resulting from obstructed salivary glandular duct system. It has also been linked to tobacco smoking and exposure to harmful radiation. Some studies associated the development of this neoplasm to continuous use of mobile phones for long periods, but this risk remains controversial.
Diagnosis begins with physical examination and localization of the mass. If abnormal growth is suspected, the patient undergoes tissue sampling test and radiographic diagnostics.
To confirm the type of mass, tissues from the lesions are extracted either through fine needle aspiration (FNA) or core needle biopsy. FNA utilizes a small gauge needle guided by ultrasound to aspirate samples with a 90% of sensitivity in differentiating benign from malignant tissues in the cytologic studies. Larger needle is used in core needle biopsy making it more invasive but more accurate than FNA.
Radiographic imaging procedures are performed to determine the extent of mass growth and regional lymphatic tissue spread. Initially, ultrasound is indicated for superficial lesions while CT scan and magnetic resonance imaging (MRI) are indicated for the deeper and more extensive lesions.
Another less popular radiographic procedure for this case is sialography. In sialography, a special dye or contrast medium is injected into the salivary gland followed by x-ray to obtain images of the tumor.
Pleomorphic Adenoma Surgery
Surgical resection of the affected salivary gland remains to be the mainstream management of pleomorphic adenoma. Complete excision or removal of the gland is commonly done for submandibular – sublingual and minor salivary gland tumors.
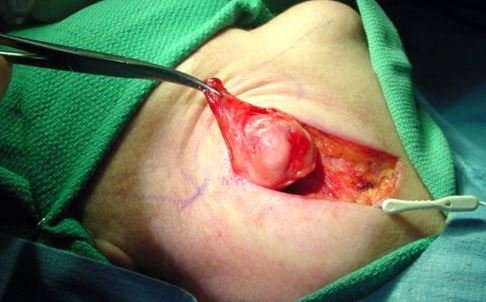
For parotid neoplasm, the superficial portion of the gland located laterally to the facial nerve, is resected. Total parotidectomy or removal of the entire parotid gland, is considered by the healthcare provider to prevent exacerbation in cases with high probability of recurrence.
If regional lymph node involvement is established, the case may necessitate neck dissection to remove the growth.
Certain complications may arise from the surgical procedure when adjacent nerves are severed. Injury to the facial nerve results to facial paralysis. The tongue could also be paralyzed when the hypoglossal or lingual nerves are damaged.
Frey’s Syndrome can occur in post parotid surgery if the autonomic nerve pathway in the area of the procedure is disturbed. This condition manifests with reddened cheeks and abnormal sweating triggered by eating or perceiving food that induces salivation.
Pleomorphic Adenoma Treatment
Aside from surgery, radiation therapy is prescribed to selected cases in order to suppress the cellular activity of the mass and prevent recurrence. Common side effects of this regimen include xerostomia or dryness of the mouth and oral mucositis or mouth membrane inflammation.
Chemotherapy, unlike other cancers, is not a modality of treatment for this disease. There is no established protocol yet for the use of chemo drugs for benign salivary tumors.
References
Alves FA, Perez DC, Almeida OP, Lopes MA, Kowalski LP. Pleomorphic Adenoma of the Submandibular Gland: Clinicopathological and Immunohistochemical Features of 60 Cases in Brazil. Arch Otolaryngol Head Neck Surg. 2002;128(12):1400-1403. doi:10.1001/archotol.128.12.1400. Retrieved from http://archotol.jamanetwork.com/article.aspx?articleid=483173
American cancer society (2014). What is salivary gland cancer? American Cancer Society. Retrieved from http://www.cancer.org/cancer/salivaryglandcancer/detailedguide/salivary-gland-cancer-what-is-salivary-gland-cancer
Eveson J, Kusafuka K, Stenman G, Nagao T. (2007).Tumours of the salivary glands. Pathology and Genetics of Head and Neck Tumors. Lyon, France: IARC Press. 254- 258.
Knipe, H., and Gaillard, F. (2015). Pleomorphic adenoma of the salivary glands. Radiopaedia.org,UBM Medica Network. Retrieved from http://radiopaedia.org/articles/pleomorphic-adenoma-of-the-salivary-glands
Patient.(2015). Salivary gland tumors. Patient. Egton Medical Information Systems Limited, England. Retrieved from http://www.patient.co.uk/doctor/salivary-gland-tumours
Phelps, P. (2015). Pleomorphic adenoma (benign mixed tumor) of the lacrimal gland. Eyewiki. Retrieved from http://eyewiki.aao.org/Pleomorphic_adenoma_%28benign_mixed_tumor%29_of_the_lacrimal_gland
Rai, S., Sodhi, S. P. S., & Sandhu, S. V. (2011). Pleomorphic adenoma of submandibular gland: An uncommon occurrence. National Journal of Maxillofacial Surgery, 2(1), 66–68. doi:10.4103/0975-5950.85857. Retrieved from http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3304236/
Said, S. (2015). Pathology of pleomorphic adenoma. Medscape. WebMD LLC. Retrieved from http://emedicine.medscape.com/article/1630933-overview
Thoeny, H. (2007). Imaging of salivary gland tumours. Cancer Imaging. Pubmed. 7: 52-62.doi:10.1102/1470-7330.2007.0008
Similar Posts:
- Adrenal Adenoma
- Acinic Cell Carcinoma
- Sebaceous Adenoma – Causes, Symptoms, Treatment, Pictures
- Pituitary Gland Tumor
- Pineal Gland Tumor
- Syringoma – Treatment, Removal, Pictures, Causes, Surgery, Prevention
- Sessile Polyp






Leave a Reply