Definition
Cystic hygroma abbreviated as CH is an abnormal growth often considered as a congenital multiloculated lesion in the lymphatic system that may arise in any location of the body; although it has been noted mostly in the head, the neck and the armpit sites.
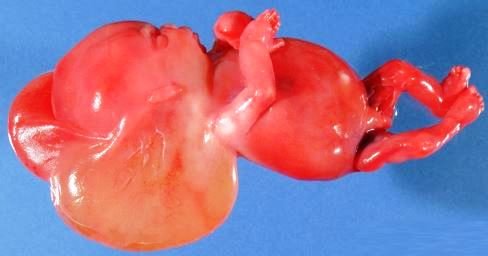
Large cyst-like cavities with lymph discharges are contained by a cystic hygroma which is made up of a watery fluid that is circulating throughout the lymphatic system. It is a benign condition, but it can be disfiguring an affected person.
CH is also referred to as a macrocystic lymphatic malformation or a cystic lymphangioma. This problem usually forms itself at the time of the pregnancy while the baby is still inside a woman’s uterus, or it can also develop after the time of delivery.
It is generally affecting children and in some rare cases, it is noted to be among adult individuals. CH simply means a water tumor due to its sponge-like collection of an abnormal growth that is filled with some clear type of lymphatic fluid.
There are two types of CH and these are:
- Macrocystic lymphatic malformations, which are the large cysts
- Microcystic lymphatic malformations, pertain with the small cysts
A person who is diagnosed to have the CH may present with only one kind of the malformations, or may have a mixture of both the macrocystic and microcystic malformations. It is found to occur approximately in 1% among the fetuses, commonly between the 9th week until the 16th week age of gestation.
CH has been known to be associated with fetal hydrops, nuchal lymphangioma, Turner syndrome, Noonan syndrome, Trisomy 13, Trisomy 18, congenital cardiac anomalies, Cornelia de Lange Syndrome, fetal alcohol syndrome, Apert syndrome, Fryns syndrome, limb hypertrophy, Pena Shokeir syndrome, and lethal multiple pterygium syndrome.
Symptoms of Cystic Hygroma
Cystic hygromas are not clearly visible at the moment of birth of a newborn baby. It can be visible as the child grows older and the CH can also get larger and bigger as well in time. Most of the cystic hygromas are noticeable as the child reaches 2 years old.
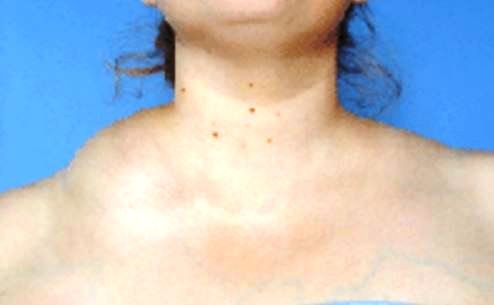
The main clinical manifestation of CH is the presence of a non-tender compressible lump that is soft, usually located on the neck, which is referring to the common neck growth. It can also develop in other body areas such as the head, armpits, groin, buttocks and even underneath the trunk skin or the limbs of a patient.
Other symptoms among infants or children are:
- Feeling of pain
- Lump in the mouth, neck, cheek or tongue
- Dyspnea
- Infection
- Bleeding problem like in hemorrhage
- Respiratory compromise
CH varies in size accordingly from a smaller size into a bigger size, just like a similar size of the child’s head. Large-sized hygromas can interfere with movements leading to some difficulties, or it can affect some daily routine activities.
Pathology
Cystic hygroma can arise, either due to a genetic syndrome or as a result of some environmental factors. CH is observed among children with an existing genetic or chromosomal abnormality. There might be one or more abnormal growths at the specific period when the diagnosis is being made.
Common genetic conditions which are linked with the development of CH:
- Turner’s syndrome, in which a female child has only one chromosome, instead of normally having two
- Trisomy 13, 18 or 21, where an affected child has the extra chromosomal copy
- Noonan syndrome ends up to a mutation in one of the seven particular genes involved
Common environmental factors leading to CH:
- Exposure to viral infections which are passed from the mother going to the baby during the pregnancy period
- Exposure to the use of drugs or alcohol drinking by the mother at the time of pregnancy
Diagnosis
Physicians recommend the following procedures:
- Antenatal ultrasound to detect the presence of CH
- Amniocentesis can be ordered after CH is detected through an ultrasound; this is important in assessing for the presence of genetic abnormalities with the growing fetus
- Fluorescent in-situ hybridization (FISH) used to evaluate CH during a prenatal chromosomal analysis
Imaging studies to specify the nature of the presenting cystic mass of the neck:
- Magnetic resonance imaging gives the best tissue detail about an existing CH
- Ultrasonography shows the relationship of CH with its surrounding
- Computed tomography enhances the visualization of the cystic wall and its surrounding structures
Treatment
Cystic hygromas do not need any treatment during pregnancy instead; attending physicians will perform close monitoring of fetal status.
Surgery is the best option to remove all of the CH after it is noted at the time of birth.
Shrinking methods for large CH that cannot be removed by surgery due to its risks:
- Use of sclerotherapy
- Use of chemotherapy
- Use of radiation therapy
- Utilization of steroid medications as prescribed
Prognosis
Chromosomal abnormalities are usually seen among fetuses who have CH. If in some instances CH resolves on its own by the 20th week of the pregnancy, and upon assessment the baby has the normal chromosomes, future outcomes are considered good. On the other hand, if it does not resolve on its own, then there is that great tendency that the fetus can encounter serious type of medical complications.
References
- Clinical presentation Ultrasound Pictures, Causes, Prognosis, Symptoms at http://radiopaedia.org/articles/cystic-hygroma-1
- http://www.healthline.com/health/cystic-hygroma#Treatments5
- http://emedicine.medscape.com/article/994055-workup#c4
- Sanhal CY, Mendilcioglu I, Ozekinci M, Yakut S, Merdun Z, Simsek M, et al (2014 Sep). Prenatal management, pregnancy and pediatric outcomes in fetuses with septated cystic hygroma. Braz J Med Biol Res. 47(9):799-803.
- Shergill A, John P, Amaral JG (2012 Sep). Doxycycline sclerotherapy in children with lymphatic malformations: outcomes, complications and clinical efficacy. Pediatr Radiol. 42(9):1080-8.
- Perkins JA, Manning SC, Tempero RM, Cunningham MJ, Edmonds JL Jr, Hoffer FA, et al (2010 Jun). Lymphatic malformations: current cellular and clinical investigations. Otolaryngol Head Neck Surg. 142(6):789-94.
Similar Posts:
- Partial Molar Pregnancy – Pictures, Symptoms, Treatment
- Choriocarcinoma – Symptoms, Prognosis, Treatment, Diagnosis
- Ovarian Teratoma
- Rhabdomyosarcoma
- Ewing’s Sarcoma – Prognosis, Survival Rate, Symptoms, Treatment
- Childhood Leukemia
- Rhabdoid Tumor






Leave a Reply