What Is Hepatoblastoma?
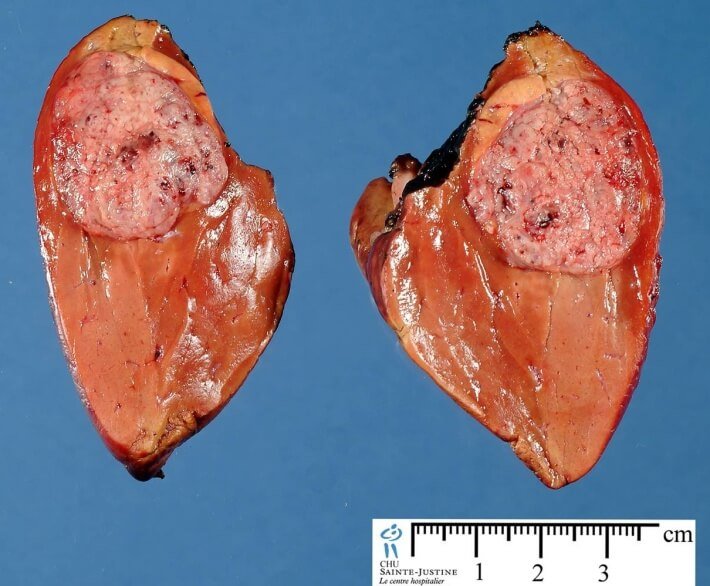
A hepatoblastoma is a cancerous tumor of the liver. They usually occur in children under three years of age. Hepatoblastomas are the most common kinds of liver cancer in children.
Hepatoblastomas account for about 1% of pediatric cancers and they account for 79% of pediatric liver cancers. The cause of hepatoblastomas is unknown. They have been associated with Beckwith-Weidemann syndrome, low birth weights, familial adenomatosis polypi and hemihypertrophy.
Hepatoblastomas occur most frequently in babies. Caucasian babies are five times more likely than African babies to get hepatoblastomas. African babies tend to have worse outcomes than other babies. Males are more frequently affected than females. [1, 2, 3, 4]
Symptoms
- Painless lump in the abdomen
- Pain in the abdomen
- Swelling in the abdomen
- Weight loss
- Appetite loss
- Ruptured tumors will result in acute abdominal symptoms
- Early puberty in males (penile and testicular enlargement without pubic hair)
- Nausea
- Vomiting
- Hemihypertrophy (one side of the body grows more than the other)
- Beckwith-Weidemann syndrome features
- Clubfoot
- Ductus arteriosus fails to close after birth
- Congenital heart disorders like tetralogy of fallot
- Rare GI disorders like extra hepatic biliary atresia
- Kidney anomalies
- Cleft palate
- Malformations of the ears
- Goldenhar syndrome
- Prader-Willi syndrome
- Congenital diverticulum
- Simpson-Golabi-Behmel syndrome
- Sotos syndrome
- Osteopenia
- Anemia and low platelet counts
- AFP levels increased [1, 2, 3]
Diagnosis
The doctor will use diagnostic testing to learn more if they suspect liver cancer. Blood tests will be completed looking at the complete blood count levels, liver function tests and serum tumor marker test. An abdominal x-ray, ultrasound, MRI and/or CT scan will be ordered to look for a mass in the abdomen.
MRI and CT scans can also help in staging any cancer that has been found and to look for any metastases. A biopsy of a tumor that is found will help diagnose cancer or rule it out. Bone scans can help look for metastases in the bones. [1, 2]
Staging
-
Pre-surgical
- Stage One– cancer in one section of the liver, three sections that are next to each other do not have cancer
- Stage Two– cancer in one or two sections of the liver, two sections that are next to each other do not have cancer
- Stage Three– one of these are true: 1) cancer in three sections of the liver and one does not have cancer 2) cancer in two sections of the liver AND two sections that are not next to each other do not have cancer
- Stage Four– cancer in all four sections of the liver
Surgical
- Stage One– cancer only in liver and all of it was removed by surgery
- Stage Two– cancer only in liver and all of it that could be seen without a microscope was removed by surgery, small amount of cancer remains or was spilled before/during surgery
- Stage Three– one of these are true: 1) cancer cannot be removed via surgery 2) cancer that can be seen without a microscope remains after surgery 3) cancer spread to lymph nodes
- Stage Four– cancer spread to other parts of the body
Recurrent
- Cancer that has been treated in the past but has come back [1]
Differential Diagnosis
- Hemangioma
- Hemangioendothelioma
- Hamartoma
- Hepatocellular carcinoma [3]
Treatment
There are standard treatments and clinical trial treatments for hepatoblastomas. Sometimes the doctor will want the patient to wait and watch the tumor until symptoms change.
Another option for liver cancer is chemotherapy. Strong anti-cancer drugs called chemotherapy can be given orally or by injection. Children with liver cancer are treated with chemo-embolization of the hepatic artery. The anti-cancer medication is mixed with another substance and is injected into the hepatic artery.
This combination blocks the artery stopping blood flow to the cancer. Most of the chemotherapy is trapped near the cancer and only small amounts can get through to other parts of the body. Sometimes this blockage is temporary and sometimes it is permanent. The cancer is prevented from getting nutrients and oxygen to grow. The liver can still get blood flow from the hepatic portal vein.
Another option is surgery to remove the cancer whenever possible. 1/3 of patients will have a complete resection at diagnosis. 60% of patients will have tumors that cannot be resected completely at diagnosis. 10% percent of patients will have metastases at diagnosis.
Cryosurgery freezes and destroys the cancer. A partial hepatectomy removes part of the liver. A total hepatectomy removes all of the liver and it is replaced by a donor liver. A liver transplant is only possible if the cancer has not spread beyond the liver and as long as a donor liver is available. A resection of metastases is a surgery to remove metastases that have spread beyond the liver.
Radiation therapy uses radiation or high energy x-rays to destroy cancer cells. Another option is percutaneous ethanol injections which can kill cancer cells as well. [1, 2]
 Life Expectancy
Life Expectancy
Liver transplants offer long term disease free survival with an 80% survival rate. Liver transplants with complete cancer removal and chemotherapy have a survival rate close to 100%.
Metastases, non-resectable tumors and recurrent cancers are poor survival indicators. Other morbidity can come from precancerous conditions, surgery complications and toxicity of chemotherapy. [2, 3, 4]
Patients with Hepatoblastoma
Reference List:
- Children’s Cancer Research Fund, Available from: http://www.childrenscancer.org/main/liver_cancer_hepatoblastoma/
- Emedicine Medscape, Available from: http://emedicine.medscape.com/article/986802
- The Oncologist, Available from: http://theoncologist.alphamedpress.org/content/5/6/445.long
- Wikipedia, Available from: https://en.wikipedia.org/wiki/Hepatoblastoma
- Humpath.com, Available from: http://www.humpath.com/spip.php?article2775
- Eastern Daily Press, Available from: http://www.edp24.co.uk/news/health/a_one_in_18
Similar Posts:
- Stage 4 Liver Cancer (End Stage) – Life Expectancy, Survival Rate
- Klatskin Tumor
- Choriocarcinoma – Symptoms, Prognosis, Treatment, Diagnosis
- Urethral Cancer
- Vaginal Cancer – Symptoms, Signs, Pictures, Treatment, Causes
- Choroidal Melanoma
- Duodenal Cancer – Symptoms, Prognosis, Survival Rate and Treatment








Leave a Reply