What is Krukenberg Tumor?
Krukenberg tumor is a metastatic cancerous development spread from stomach to ovary. The development of the Krukenberg Tumor is not from general gastric cancer, but it is a specific form of cancerous growth arises from signet ring cell carcinoma of the stomach and spread to adenocarcinoma of the ovary.
The primary place of development of the Krukenberg tumor is the stomach, but other primary sites of tumor progression are from the colon, appendix, and breast. In a rare instance, krukenberg tumor can also originate from the biliary tract, gallbladder, pancreas, small intestine, urinary bladder, ampulla of Vater and cervix1,2.
History
The name of this metastatic tumor is derived from its discoverer, Friedrich Ernst Krukenberg, who first published 5 case history of krukenberg tumor in the year 1896. During this time period, Friedrich Ernst Krukenberg worked as a student in German laboratory3.
Incidence
A few years back, the predominance of Krukenberg tumor is rare and only 1% to 2% incidence is found as krukenberg tumor comparing with all instance of ovarian tumors. But recent days, krukenberg tumor incidence become higher and it accounts almost 5% to 20% of all other types of metastatic ovarian cancer3,4.
Symptoms
Initially, Krukenberg tumor is asymptomatic or mild and non-specific. But in a later stage, the symptoms become specific as the size of the tumor become larger.
- Feeling of lump in the abdomen and that causes abdominal distention
- Affected individual can feel a large lump present in the lower region of the abdomen.
- Bloating cause feeling of gastrointestinal discomfort
- Lower abdominal pain arises
- Peritoneal cavity filled due to fluid accumulation and inflammation occur in abdominal wall (ascites)
- Reactive ovarian stroma and stimulates hormone secretion leads vaginal bleeding
- Irregular period
- Hirsuitism
- Sporadic virilization
- Pain during sexual intercourse
- Unexplained lethargy
- Bowel habit become alter and patients usually suffering from constipation2, 5, 6
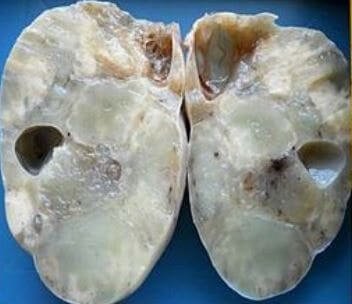
Pathology
Krukenberg tumors have capsular smooth surface without adhesions or peritoneal deposition. Histological analysis showed that epithelial and stromal are two component presents in Krukenberg tumor. Mucin-laden signet ring cells with eccentric hyperchromatic nuclei are present in the epithelial component. Most of the tumor cells have central large vacuole with a droplet of mucin at the central to paracentral eosinophilic body. Eosinophilic and granular cytoplasm present in the cytoplasm of the signet ring cells. In some tumor cells, mucin vacuole is not present4.
Diagnosis
- The diagnosis of Krukenberg Tumor is usually incidental mainly after diagnosis of stomach cancer. CT staging scan detects Krukenberg Tumor at the late stage of malignancy. Krukenberg Tumor is usually unilateral, but in rare instance both the ovaries are affected.
- In hematological testing, the elevated amount of CA125 tumor marker may indicate the presence Krukenberg Tumor. But this test is not considered as a confirmatory test, as the elevation of CA125 tumor marker is found in another type of disease condition.
- A tissue biopsy is provided a confirmatory result.
- If no history of stomach cancer or no evidence supports the presence of gastric cancer then further tests required to exclude the possibility of the presence of breast cancer or colon cancer. mammography is recommended for breast cancer, whereas colonoscopy is recommended to check colon2.
Treatment
- No optimum treatment plan is determined for treating Krukenberg tumors. Krukenberg tumor is a non-curable disease. Chemotherapy and radiation therapy do not provide improved survival rate4.
- The available treatment options also include invasive surgical resection based. Surgical resection is preferable when no other malignant tumor associated with Krukenberg tumors7.
- Some prefer to conduct bilateral oophorectomy during primary tumor surgery for prophylactic purposes8.
- Recent days, targeted chemotherapy and surgical debulking are applied to get more promising result9.
- The assistance of palliative care unit is required at the last stage2.
Survival Rate & Prognosis
The survival rate is poor in patients suffering from Krukenberg tumors. The medical literature mentioned that usually patient died with 2 years and average month of survival is considered only 14 months. Disease diagnosis and initiates treatment management have an impact on the prognosis of Krukenberg tumors and that also alter survival rate. It has been observed that metastasis nature of primary tumor identification cause poor prognosis, whereas if the primary tumor remains undiagnosed or covert, then that worsen the prognosis.
The treatment plan is very crucial to get increased survival rate. medical research showed that preliminary surgical removal of primary carcinoma followed with surgery on the ovarian tumor provide better survival than simultaneous surgery or first ovarian tumor removal and later surgical intervention of primary carcinoma provides a low rate of survival.
The prognosis of the disease also depends upon the origin of cancer. The survival prognosis is poor in ovarian metastases of gastric carcinoma in comparing with breast and colorectal carcinoma4, 10.
References
- Dr. Jeremy Jones, Dr. Yuranga Weerakkody et al.; Krukenberg tumour; Radiopaedia.org; Online available at https://radiopaedia.org/articles/krukenberg-tumour-1
- Krukenberg Tumor; Stomach Cancer; Online available at http://www.mystomachcancersymptoms.com/krukenberg-tumor.html#1
- Young RH. From Krukenberg to today: the ever present problems posed by metastatic tumors in the ovary. Part I: historical perspective, general principles, mucinous tumors including the Krukenberg tumor. Adv Anat Pathol. 2006;13:205–227.
- Osama M. Al-Agha, Anthony D. Nicastri; An In-depth Look at Krukenberg Tumor An Overview; Arch Pathol Lab Med—Vol 130, November 2006; http://www.archivesofpathology.org/doi/pdf/10.1043/1543-2165(2006)130%5B1725:AILAKT%5D2.0.CO%3B2
- Kiyokawa T, Young RH, Scully RE. Krukenberg tumors of the ovary: a clinicopathologic analysis of 120 cases with emphasis on their variable pathologic manifestations. Am J Surg Pathol. 2006;30:277–299.
- Papakonstantinou E, Liapis A, Kairi-Vassilatou E, Iavazzo C, Kleanthis CK, Kondi-Pafiti A. Virilizing ovarian Krukenberg tumor in a 27-year-old pregnant woman: a case report and literature review. Eur J Gynaecol Oncol. 2011;32:331–333.
- Novak E, Gray LA. Krukenberg tumors of the ovary: clinical and pathological study of 21 cases. Surg Gynecol Obstet. 1938;66:157–167.
- McGill FM, Ritter DB, Rickard CS, Kaleya RN. Krukenberg tumors: can management be improved? Gynecol Obstet Invest. 1999;48:61–65.
- Germann N, Gross-Goupil M, Wasserman E, Emile JF, Misset JL, Reynes M: The chemotherapy of metastatic gastric adenocarcinomas with hypersecretion of alpha-fetoprotein or beta-human chorionic gonadotropin: report of two cases. Ann Oncol 2002,13(4):632–636. 10.1093/annonc/mdf026
- Demopoulos RI, Touger L, Dubin N. Secondary ovarian carcinoma: a clinical and pathological evaluation. Int J Gynecol Pathol. 1987;6:166–175.
Similar Posts:
- Serous Cystadenoma
- Triple Negative Breast Cancer
- Ovarian Teratoma
- HER2 Positive Breast Cancer
- DCIS Breast Cancer
- Brenner Tumor
- Germ Cell Cancer – Symptoms, Survival Rate & Prognosis






Leave a Reply