What is an Adrenal Gland Tumor?
An adrenal gland tumor is a growth in the adrenal gland. A tumor starts when healthy cells change and grow wildly forming a mass. An adrenal gland tumor can be cancerous (malignant) or non-cancerous (benign). If an adrenal gland tumor is malignant then it has the chance to grow and spread to other areas of the body.
If an adrenal gland tumor is benign then it can grow but will not spread to other body areas. A functioning tumor produces too many hormones. A non-functioning tumor does not produce any hormones. A primary adrenal gland tumor starts in the adrenal gland. Metastasis occurs when cancer spreads from another area. A primary adrenal gland tumor is rare. Most adrenal gland tumors are benign.
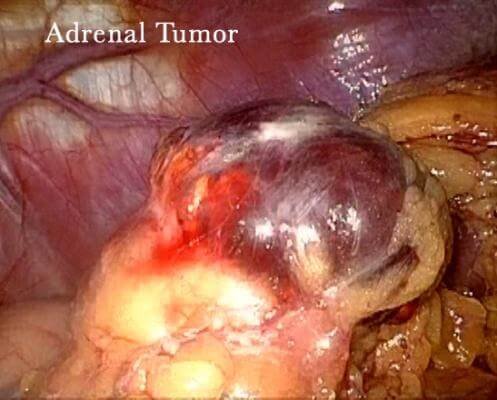
Adenoma is the most common kind of adrenal gland tumor. This kind of tumor is non-cancerous and non-functioning. It grows in the adrenal cortex. This type of tumor usually does not cause symptoms. If it stays small it usually does not need treatment.
Adenomas are also known as adrenocortical adenoma. This kind of tumor is seen in adults around middle age and older. Women tend to be diagnosed more often with this type of tumor than men.
Adrenocortical carcinoma
this is rare but it is also the most common type of adrenal gland cancer. Adrenocortical carcinoma is also known as cortical carcinoma. Four to twelve out of one million people develop this kind of cancer each year. It grows in the adrenal cortex. It can be functioning or non-functioning. These kinds of cancerous adrenal gland tumors are usually large in size but the benign tumors are usually small.
More women than men have a diagnosis of this kind of tumor. Adrenocortical carcinoma tends to affect the right adrenal gland more often than the left. Estimates note this type of cancer is seen in about 200 to 500 people each year in the USA.
Neuroblastoma
this is a childhood cancer that grows in the adrenal medulla. Neuroblasts are immature nerve cells that are found in unborn babies. Normal neuroblasts mature in adrenal medulla cells in the adrenal glands. Neuroblastoma comes from neuroblasts that do not mature properly.
Pheochromocytoma
this is an adrenal gland tumor that most often starts growing in the adrenal medulla. These tumors come from the neuroendocrine cells. It is a rare tumor that increases production of adrenaline and noradrenaline which causes increased blood pressure and heart rate. It is usually benign but it can be life threatening if too much adrenaline is produced. The presence of metastases is the only reliable indicator of malignancy for pheochromocytomas.
Both adrenal glands are affected in about ten percent of cases. Pheochromocytoma is more likely to occur in people with a genetic disorder. This kind of adrenal gland disorder affects men and women equally.
Myelolipomas
there are very rare benign tumors that can start in the adrenal glands. They are made up of fat and blood forming tissues.
Cysts and pseudo-cysts
that can start to grow in the adrenal glands as well. They are subdivided into four sub types: endothelial, pseudo-cyst, epithelial and parasitic.
Adenomatoid tumors
These are rare benign tumors of the adrenal glands. Lymphoma is a rare tumor that can start in the adrenal glands. Only about one hundred cases of this type of tumor has been reported. [1, 2]
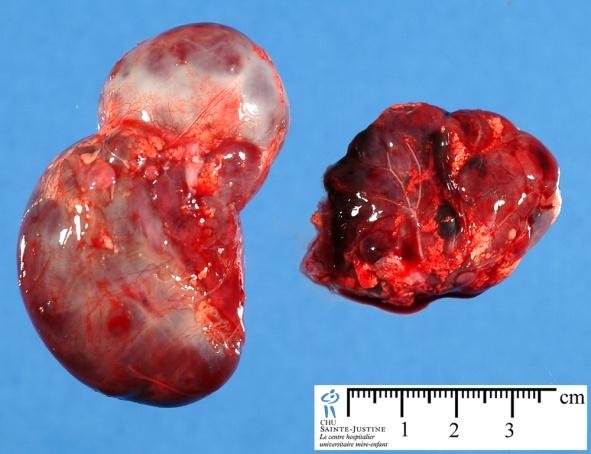
Adrenal Gland Purpose & Functions
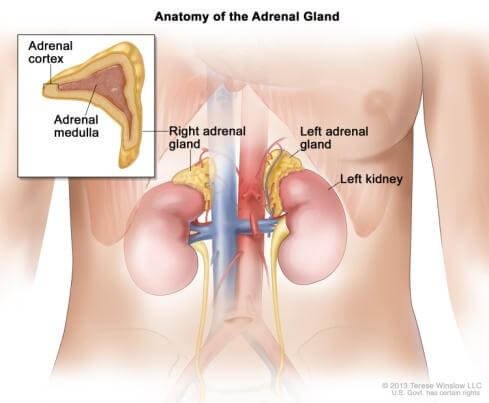
Each person has two adrenal glands. They are located over top the kidneys. They are small and yellow in color. Adrenal glands normally weigh around ten grams. Adrenal glands are a part of the body’s endocrine system. The endocrine system is responsible for producing hormones.
The adrenal glands are made up of two parts: the adrenal cortex and the adrenal medulla. The adrenal cortex is responsible for metabolism, blood pressure, hair growth and body shape. The adrenal cortex makes cortisol, aldosterone and DHEA. The adrenal medulla is responsible for the body’s response to stress. The adrenal medulla makes epinephrine, norepinephrine and dopamine. [2]
Risk Factors of Adrenal Tumors
The hereditary conditions that increase the risk for adrenal gland tumors are: multiple endocrine neoplasia type two, Li-Fraumeni syndrome, Von Hippel –Lindau syndrome, McCune-Albright syndrome, Cowden syndrome, neurofibromatosis type one and Carney complex. [1, 2]
Signs & Symptoms
- Usually does not produce symptoms
- If the tumor is producing excess hormones then the person may have hormone related signs and symptoms
- Can cause Conn syndrome and Cushing syndrome [1]
 Symptoms
Symptoms
- High blood pressure
- Low potassium levels
- Heart palpitations
- Anxiety
- Headaches
- Sweating
- Diabetes
- Abdominal pain
- Weight gain or weight loss
- Weakness
- Abdominal stretch marks
- Excessive hair growth
- Genitalia changes
- Acne
- Sex drive changes [2]
Pheochromocytoma Signs & Symptoms
- High blood pressure
- Orthostatic hypotension
- Headaches
- Sweating
- Fast heart rate
- Heart palpitations
- Anxiety
- Weakness
- Visual problems
- Abdominal pain or chest pain
- Diarrhea [1]
Signs & Symptoms of Cortisol Over-Production
- Moon face (round face)
- Weight gain (mostly on the collar bone and abdomen)
- Buffalo hump (lump on the neck)
- Excessive hair growth on the face/arms/chest/back in women
- Acne (after puberty)
- Stretch marks on the abdomen that are purple
- Weak muscles
- High blood sugar (in people with no risk for diabetes)
- High blood pressure
- Abnormalities with menstrual cycle
- Bruises easily
- Women can have deepening of the voice
- Swelling of sex organs
- Mood changes and depression
- Thinning bones [1, 3]
 Moon face [9]
Moon face [9]
Signs & Symptoms of Aldosterone Over-Production
- High blood pressure
- Weak muscles
- Muscle cramps
- Increased thirst
- Low potassium levels
- Increased urination
- Headaches in the front of the head
- Paraesthesia like numbness, tingling and pins/needles
- Heart problems
- Vision changes [1, 3]
Signs & Symptoms of Excess Androgen
- Excessive androgen in women
- Excessive hair growth on the face/arms/chest/back in women
- Acne
- Balding
- Women can have deepening of the voice
- Absence of menstruation
- Excessive androgen in men usually does not cause symptoms
- Excessive estrogen in women
- Abnormalities with menstrual cycle in pre-menopause
- Menstrual bleeding in post-menopause
- Excessive estrogen in men
- Breast enlargement
- Breast tenderness
- Decreased sex drive
- Impotence
- Puberty starts early in children [1]
Signs & Symptoms of Non Functioning Tumors
- Abdominal pain or back pain
- Full feeling in abdomen
- Lump in the abdomen
- Early satiety/feeling full earlier than normal [1]
Diagnosis
Doctors need to rule out all other possible problems before confirming an adrenal gland tumor. A physical examination and patient history will be completed. The doctor will look for signs, symptoms, risk factors, medical events and problems in the past. They will look for any personal or family history of cancer. The doctor will look at the person’s blood pressure, pulse, changes in physical appearance and look for any lumps in the abdomen.
Diagnostic testing will be completed when symptoms of an adrenal gland tumor is present. Urine testing will be ordered. A 24 hour urine collection will be utilized to look for the amount of adrenal gland hormones. Higher than normal cortisol levels found in the urine suggest the presence of an adrenal gland tumor.
Blood chemistry testing will be completed. These blood tests will show how the body organs are functioning. The doctor will be looking for low levels of potassium and renin, high cortisol levels, high aldosterone levels, high DHEAS levels, high testosterone levels, high estrogen levels, levels of FSH, ACTH levels, chromogranin levels and high epinephrine/norepinephrine levels.
A dexamethasone suppression test may be initiated. It will measure the amount of cortisol in the person’s system. The person will take a dose of dexamethasone and their blood level will be taken afterwards. If there is a tumor in the body, the cortisol level will remain high. If there is not a tumor in the body, the cortisol level will be lower than normal.
A CT scan will be performed when laboratory testing suggests there is something wrong. The CT scan will help see any tumors in the adrenal glands. It will show any growth or spreading and the extent of any tumor. The scan will also help distinguish between benign and malignant tumors based on size, margins and density.
MRI testing can be used to see any tumors, see any spread of a tumor, the extent of any tumor, size of the tumor, margins of the tumor and density of the tumor. A MIBG scan is another option for locating and diagnosing tumors. Doctors can use a MIBG scan when the tumor does not show up on a CT scan. PET scans are used as well to look for adrenal gland tumors.
Ultrasounds can look for tumors as well but it is rarely done because CT scans are more widely used. A chest x-ray can be used to look for cancer that has spread into the lungs. A bone scan can be used to look for cancer that has spread into the bones.
Biopsies are rarely done for adrenal gland tumors. A biopsy may be done if the cancer has spread outside the adrenal gland. In rare cases where the person has symptoms but the tumor does not show on the CT or MRI scan, then adrenal vein sampling can be done. [1, 2, 3]
Staging
Doctors stage cancer to best describe and classify cancer based on the extent of cancer in the body. Pheochromocytoma does not have a staging system. People with pheochromocytoma are categorized as having cancer that is localized, regional or metastatic.
Doctors use the TNM system to stage adrenocortical carcinoma. Doctors then can sub categorize the TNM data into the UICC staging system.
Tumor Nodes Metastasis System (TNM)
Primary Tumor
- TX, primary tumor can’t be assessed
- T0, no signs of primary tumor
- T1, tumor five cm or less and no growth outside the adrenal gland
- T2, tumor larger than five cm and no growth outside the adrenal gland
- T3, tumor any size and has grown into the fat surrounding the adrenal gland but not organs
- T4, tumor any size and has grown into nearby organs
Regional Lymph Nodes
- NX, regional lymph nodes can’t be assessed
- N0, no regional lymph node metastasis
- N1, regional lymph node metastasis
Distant Metastasis
- M0, No distant metastasis
- M1, distant metastasis [1]
Metastasis
All cancer cells have the potential to spread or metastasize to other parts of the body. Adrenal gland cancer can start in the adrenal glands and spread or can spread from another area that was the primary site. The most common sites for adrenal gland cancer to spread to are:
- Regional lymph nodes
- Other adrenal gland
- Kidneys
- Diaphragm
- Pancreas
- Spleen
- Large blood vessels
- Peritoneum
- Lungs
- Liver
- Bones
The most common kinds of primary cancer that can spread to the adrenal glands are:
- Lung cancer
- Breast cancer
- Malignant melanoma
- Colorectal cancer [1]
Treatment
Benign adrenal gland tumors may not cause any symptoms at all and may not need any treatment. Surgery is an option for benign tumors. A surgical endocrinologist will remove the adrenal gland(s)/tumor and part of the healthy tissue. A laparoscopic surgery is used when the tumor is small, less than five centimeters and looks benign.
The multi-disciplinary team will work with the patient to make a plan to cover the holistic health of the patient. Surgery to remove cancerous tumors is also completed by a surgical endocrinologist.
If the tumor is cancerous and is more than five centimeters in size then the surgery is done on the abdomen or back. Chemotherapy and/or radiation may be ordered by the medical oncologist, a cancer specialist.
The doctor may treat the patient with hormones to control the hormone level deficiency caused by the malfunctioning adrenal glands. Other ways doctors may treat patients with adrenal gland tumors are: palliative care, supportive care, genetic counseling, referrals to social workers, medication treatment for pain, psychological counseling, referral to dieticians and others. [2]
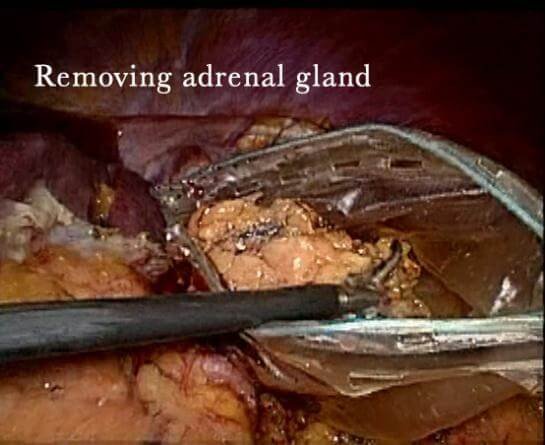
Prognosis
Adrenal gland tumors that are benign may not need treatment and may cause no symptoms. Surgical removal of benign tumors may cure the issue.
Tumors that produce hormones have better prognoses than those that do not. Tumors that over produce cortisol have a worse prognosis than other functioning tumors. Younger patients have better prognoses than older patients.
Adrenal gland tumors that are cancerous have a chance of spreading to other parts of the body. Palliative care may be the only option sometimes if the combination of treatment options does not work.
Remission of cancer can be temporary or permanent. Patients will have to work through their fears of recurrence. If the cancer recurs, then the patient will need to go through the staging process again and start new treatment plans.
The five year survival rate for endocrine gland cancer is sixty three percent in the USA. The five year survival rate for localized adrenocortical carcinoma is sixty five percent. The five year survival rate for regional adrenocortical carcinoma is forty six percent. The five year survival rate for distant adrenocortical carcinoma is nine percent.
Pheochromocytoma is mostly benign. Most people with this diagnosis are expected to live a normal life span. The metastatic pheochromocytoma five year survival rate is between forty to forty five percent.
Overall, prognosis depends on many factors including the person’s medical history, the type of cancer or tumor, cancer stage, age, characteristics of the cancer, treatments chosen and response to treatment. [1]
Reference List:
- Canadian Cancer Society, Available from: http://www.cancer.ca/en/cancer-information/cancer-type/adrenal-gland/adrenal-gland-cancer/benign-tumours/?region=bc
- Cancer.net, Available from: http://www.cancer.net/cancer-types/adrenal-gland-tumor/symptoms-and-signs
- Cancer.org, Available from: http://www.cancer.org/cancer/adrenalcorticalcancer/detailedguide/adrenal-cortical-cancer-signs-symptoms
- MD Anderson Cancer Center, Available from: https://www.mdanderson.org/cancer-types/adrenal-tumors.html
- National Cancer Institute, Available from: https://www.cancer.gov/types/adrenocortical/patient/adrenocortical-treatment-pdq
- Health Augusta University, Available from: http://www.augustahealth.org/adrenal/adrenal-surgery/adrenal-surgery-laparoscopic-adrenal-surgery AND http://www.augustahealth.org/adrenal/adrenal-surgery/adrenal-surgery-laparoscopic-adrenal-surgery
- Endocrine Pathology, Available from: http://www.endocrinepathology.nl/categories.php?parent_id=2164
- Wikipedia, Available from: https://en.wikipedia.org/wiki/Cushing’s_syndrome
- Photo Bucket, Available from: http://photobucket.com/images/prednisone%20moon%20face
Similar Posts:
- Adrenal Adenoma
- CEA Tumor Marker
- Link Between Low Testosterone and Testosterone Replacement Therapy on Cancer
- Pituitary Gland Tumor
- Pineal Gland Tumor
- Syringoma – Treatment, Removal, Pictures, Causes, Surgery, Prevention
- Acinic Cell Carcinoma






Leave a Reply